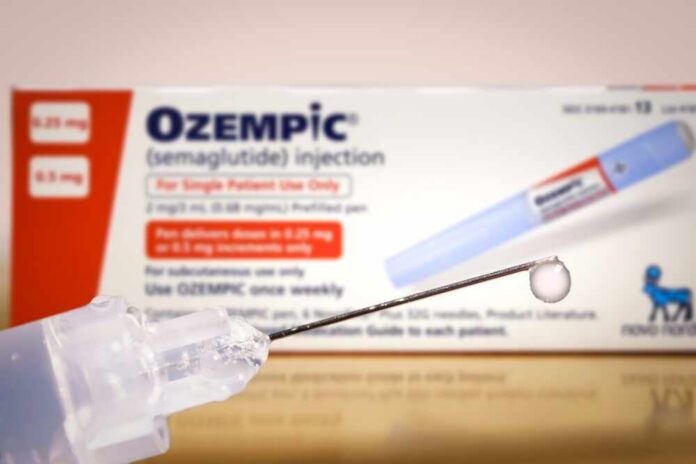
The real surprise with Ozempic and Wegovy isn’t that they work—it’s how much patients say the fine print still misses.
Quick Take
- AI analysis of real-world social media posts flagged side effects patients say don’t always show up clearly in trial summaries.
- Common issues like nausea, vomiting, and constipation may be more disruptive in everyday life than clinical language suggests.
- Doctors also watch for higher-stakes concerns: slowed stomach emptying, pancreatitis signals, and a rare but serious thyroid cancer link.
- These drugs can deliver major weight loss and potential heart-protection benefits, but long-term, lifelong-use questions remain.
Why “Hidden Side Effects” Became the New Battleground
Researchers went looking for what controlled trials often can’t capture: the messy, lived experience of people taking GLP-1 drugs such as Ozempic and Wegovy.
Instead of relying only on formal adverse-event reports, newer work used AI to scan patient discussions—especially on Reddit—where users describe symptoms in plain language, compare notes, and admit what they didn’t tell their doctor.
That method doesn’t prove causation, but it can spotlight patterns worth investigating fast.
Popular weight-loss medications linked to hidden side effects, study findshttps://t.co/N02tFFFC1E
— BREAKING NEWZ Alert (@MustReadNewz) April 15, 2026
The appeal of this approach is simple: people talk differently online than they do in an exam room. A trial might log “nausea,” while a working adult posts about nausea that ruins meetings, driving, or sleep.
A label might mention constipation, while a caregiver writes about days lost to discomfort and the spiral of remedies.
AI can cluster these descriptions into signals, then researchers can ask the right follow-up questions in more rigorous studies.
What These Drugs Do Well—and Why Millions Still Roll the Dice
GLP-1 receptor agonists started as diabetes drugs, then weight loss showed up almost like a bonus feature. The basic pitch is compelling: many users see roughly 15–20% weight loss over a year or more, numbers that can rival older surgical outcomes for some patients.
Researchers also point to broad metabolic improvements, and major cardiovascular outcomes have been anticipated, including fewer heart attacks, strokes, and cardiovascular deaths.
That upside matters to adults over 40 who have watched friends struggle with blood pressure meds, sleep apnea, aching knees, and rising A1C. Weight loss isn’t cosmetic at that point; it’s about staying employable, mobile, and independent.
The Side Effects Everyone Mentions, and the Ones That Change Medical Protocols
Most people hear about the greatest hits: nausea, vomiting, and constipation. Patient reports and news coverage suggest these can be common and sometimes intense.
The bigger practical question is not whether they occur, but whether patients can work through them without giving up. Some can. Some can’t. And when a medication’s benefit depends on staying on it, tolerability becomes a deal-breaker, not a footnote.
One concern that jumps from “unpleasant” to “procedurally important” is delayed gastric emptying. If the stomach empties more slowly, food can remain in the stomach longer than expected—relevant to sedation and endoscopy safety.
Reports describe hospitals telling patients to stop GLP-1 medications about a week before certain procedures. That kind of policy shift signals that medicine is adapting in real time, sometimes faster than formal guidance can catch up.
Pancreatitis and Thyroid Cancer: Sorting Relative Risk from Real Fear
Pancreatitis has hovered over GLP-1 drugs for years. Early warnings made it sound common; later analysis suggested the risk was likely overstated, yet not necessarily zero.
Conflicting data leaves clinicians in a familiar spot: counsel patients with humility, screen for personal risk factors, and take symptoms seriously.
Adults deserve straight talk—severe abdominal pain and persistent vomiting aren’t “normal adjustment” and shouldn’t be explained away to protect a prescription.
Thyroid cancer claims draw even more heat because they mix scary language with low base rates. Reporting describes an association where risk rises with longer use and could be roughly 50% higher than that of non-users, while thyroid cancer remains rare overall.
Common sense says two things can be true: the absolute risk may stay low, and the decision still matters—especially for patients with relevant family histories. Caution beats slogans when stakes involve cancer, however uncommon.
What Social Media “Signals” Can’t Do—and What Patients Should Demand Anyway
AI scanning of social posts can surface potential issues, but it cannot replace controlled evidence. Online communities skew toward people having problems, and self-reported symptoms can reflect diet changes, dehydration, other drugs, or underlying disease.
Still, dismissing these reports because they’re messy is a mistake. Post-market reality has a long history of surprising the medical system. The right response is disciplined curiosity: investigate signals, update guidance, and communicate plainly.
Informed consent should look less like a rushed pitch and more like a serious contract: expected benefits, realistic side effects, what “stop immediately” symptoms look like, how long therapy might last, and what the monthly bill does to a household budget.
These drugs may end up remembered as a genuine breakthrough that arrived before the rulebook was finished. The most productive takeaway isn’t panic or hype; it’s vigilance.
If you’re considering a GLP-1 medication, insist on a two-visit decision, ask about procedure timing, family cancer history, and what symptoms trigger a same-day call.
The “hidden side effects” story is really a reminder: real-world truths leak out eventually—better to plan for it up front.
Sources:
Pros, cons, and unknowns of popular weight loss drugs
Beware! New Research Reveals Unusual Side Effect Of Weight Loss Drugs Like Ozempic
New Research Uncovers Hidden Side Effects of Popular Weight-Loss Drugs
Popular weight loss medications linked to hidden side effects, study finds
Study Identifies Benefits, Risks Linked to Popular Weight-Loss Drugs